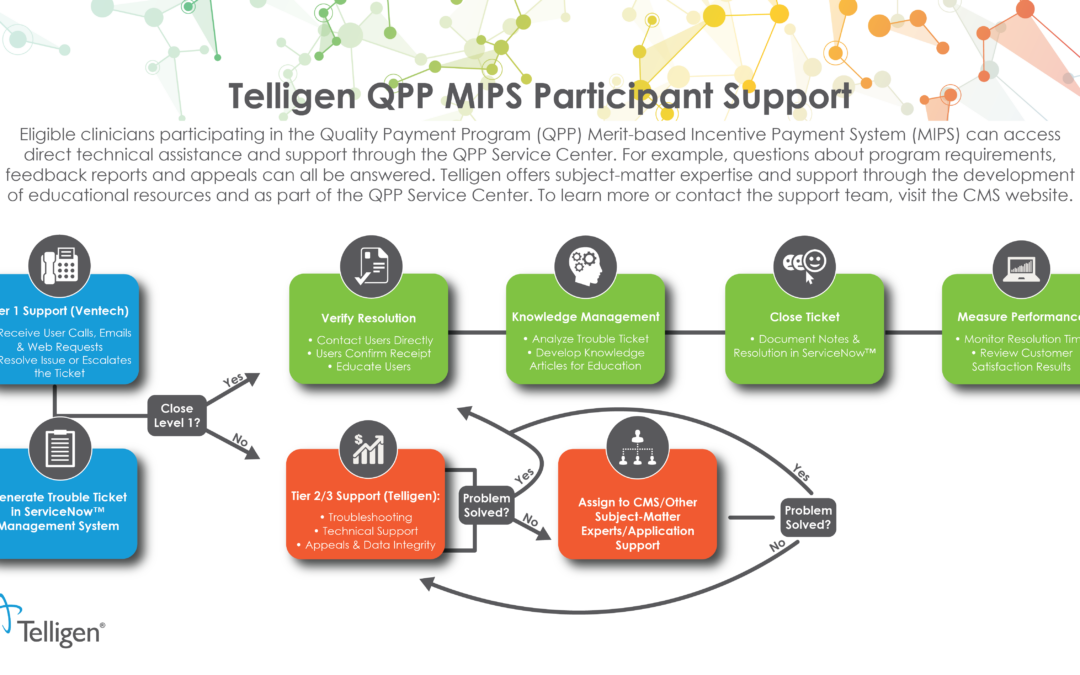
Eligible clinicians participating in the Quality Payment Program (QPP) Merit-based Incentive Payment System (MIPS) can access direct technical assistance and support through the QPP Service Center. For example, questions about program requirements, feedback reports and appeals can be answered.
Telligen provides tier 2 and 3 customer service support to QPP MIPS participants, offering subject-matter expertise and technical assistance.
As the highest tier support for QPP MIPS, we participate in program increment planning sessions with the product developers and the Centers for Medicare & Medicaid Services (CMS) every 12 weeks, creating a feedback loop from the customer service center to developers and CMS leadership:
- Customers work with QPP MIPS Service Center to resolve their issues.
- Telligen subject-matter experts attend the program increment sessions to inform CMS, product developers, and communications teams what they hear directly from the customers.
- Decisions made about the next program increment based on feedback they hear from Telligen subject-matter experts.
To learn more or contact the support team, visit the CMS website.