Utilization management
The Care Members Need, When They Need It.
what we do
Every dollar counts when you are trying to control health plan expenses. Researchers estimate about 25% of all US healthcare spending is wasteful, according to a 2019 study. Telligen’s Utilization Management program makes sure your members get the evidence-based medical care they need.
Utilization Management Services include:
Inpatient Review
- Medical
- Surgical
- Behavioral Health
- Discharge Planning
Outpatient Review
- Procedures
- Diagnostic Imaging
- Durable Medical Equipment
- Behavioral Health
Other Services
- Specialty Reviews
- Imaging Redirection
- External Review
- Skilled Nursing
- Residential Facilities
“We evaluate healthcare services for medical necessity to ensure your members get the care they need at the right time, the right place and for the best value.”
Contact a Health & Well-Being Expert Today!
how we do it
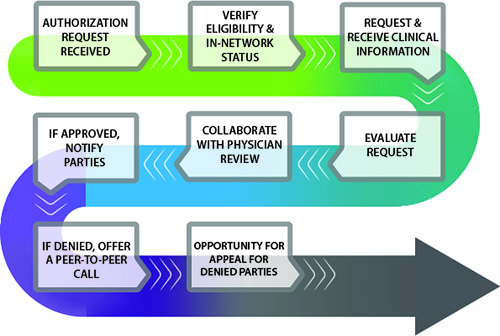
Telligen’s comprehensive Utilization Management program consists of a collaborative process between Telligen’s clinical nurses and providers. We believe our call center provides more than the typical call center. We don’t just start the review process; we verify that a review is required, create a case, facilitate transfer to a nurse to provide the clinical expertise and get the decision in one call. Healthcare services are evaluated for medical necessity, appropriateness and efficiency of use based on clinical information, evidence-based criteria and physician support. This promotes care delivery at the right time, right place and for the best value under the provisions of the applicable health benefit plan.
Success Story
The Issue: A Midwest client with nearly 70,000 members was facing rising healthcare costs year after year; yet their members’ health status was declining.
Telligen’s Role: Through Telligen’s Utilization Management program, the client was able to ensure that services were being provided based on evidence-based guidelines, delivered in the appropriate setting and medically necessary. This helped the client eliminate unnecessary services and maximize health plan savings, saving the client over $33 million on UM costs over 4 years.