Utilization management
Better Outcomes. Better Care. Lower Costs.
what we do
Telligen’s Utilization Management professionals evaluate appropriateness of services to ensure members receive the right care, in the right place, at the right time and in the right setting.
We have programs covering inpatient, outpatient and specialty services using state-specific criteria and automated review processes across our state contracts. This includes medical/surgical services and/or admissions, acute psychiatric admissions, genetic testing, and inpatient rehabilitation.
“You are the quickest and best submission process and I believe the industry standard.”
Contact a State Medicaid Solutions Expert Today!
how we do it
Telligen efficiently manages the UM review process to promote quality of care and eliminate unnecessary services. Our solution relieves the administrative burden for providers and staff while managing healthcare costs for our clients.
Our proprietary software application, Qualitrac™, is designed to interface with any third-party MMIS vendor/proprietary systems, providing seamless and secure transfer of participant, provider and claims data at on-demand intervals.
At the hub of Qualitrac is our Enterprise Data Management system, which processes, validates, and maps the data.
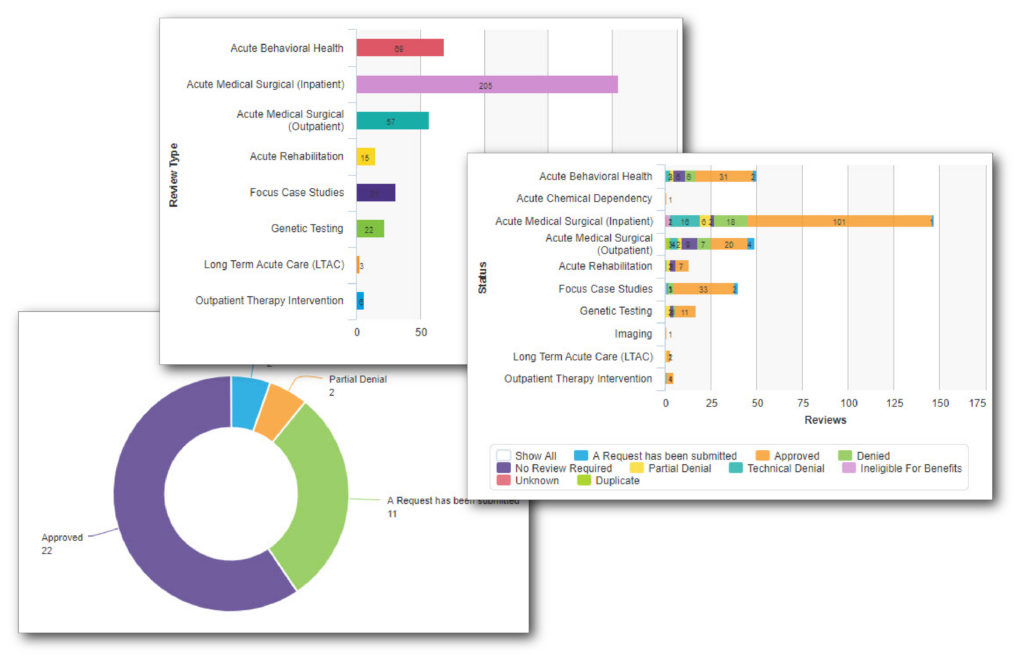
Clients can generate and review reports on their population(s) via the dashboards that are integrated into Qualitrac.
success story
Client & Program: Maryland Medicaid Utilization Control (UC) of Selected Hospital, Nursing Facility, and Home and Community Based Services, Maryland Department of Health (MDH)
Description: Designed and implemented the performance of in-home, comprehensive assessments for both adults and children. Conduct retrospective compliance reviews of Level I PASRR Reviews. Prior authorization and retrospective utilization reviews across a variety of clinical settings.
Result:
- Produced and completed an average ROI of $4 in state savings for every $1 in expenses
- Complete an average of 10,000 reviews per month for more than 18 different services
- Implemented provider portal to reduce administrative burden; improve efficiency

state solutions

assessments

care management

quality & performance improvement

quality measurement & reporting

