 Healthcare Intelligence is a new Telligen content series dedicated to exploring the latest trends, news and research across the entire spectrum of health and wellness.
Healthcare Intelligence is a new Telligen content series dedicated to exploring the latest trends, news and research across the entire spectrum of health and wellness.
There is a growing need in healthcare for innovative solutions that can streamline various processes and improve patient outcomes. One such solution is the use of Natural Language Processing-enabled (NLP) chatbots in healthcare, which can help healthcare providers check the status of prior authorization reviews. In this article, we will explore how Telligen uses NLP-enabled chatbots to improve prior authorization experience for providers, resulting in fewer delays and reduced provider burden.
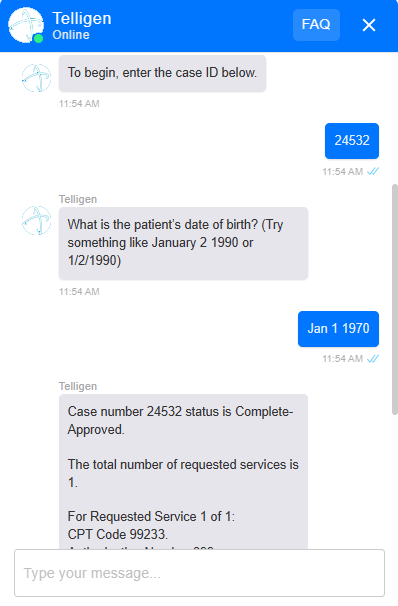
An example of Telligen’s chatbot capabilities in action (demo data displayed)
Prior authorization is a critical process that healthcare providers must perform in order to ensure that patients are receiving necessary medical treatments and procedures at the right time and setting. This process involves obtaining approval from insurance companies or other healthcare payers before providing certain services or medications. Unfortunately, despite continued advancements to streamline the prior authorization process, it can still be time-consuming and complicated, which can lead to delays in patients getting the care they need.
This is where NLP-enabled chatbots can help. A chatbot is a form of artificial intelligence-powered software that can communicate with users through a messaging interface. By using natural language processing and machine learning algorithms, chatbots can understand the context of a conversation and provide appropriate responses.
In the context of prior authorization, NLP-enabled chatbots can help healthcare providers check the status of a prior authorization request by interacting with the payer’s system. For example, the chatbot can ask the healthcare provider for the patient’s review ID and date of birth. Using this information, the chatbot can then access Telligen’s Qualitrac system and provide the healthcare provider with real-time updates on the status of the prior authorization request.
Workflow
The diagram below shows how Telligen is employing Amazon Lex Chatbot to get status queries of prior authorization reviews.
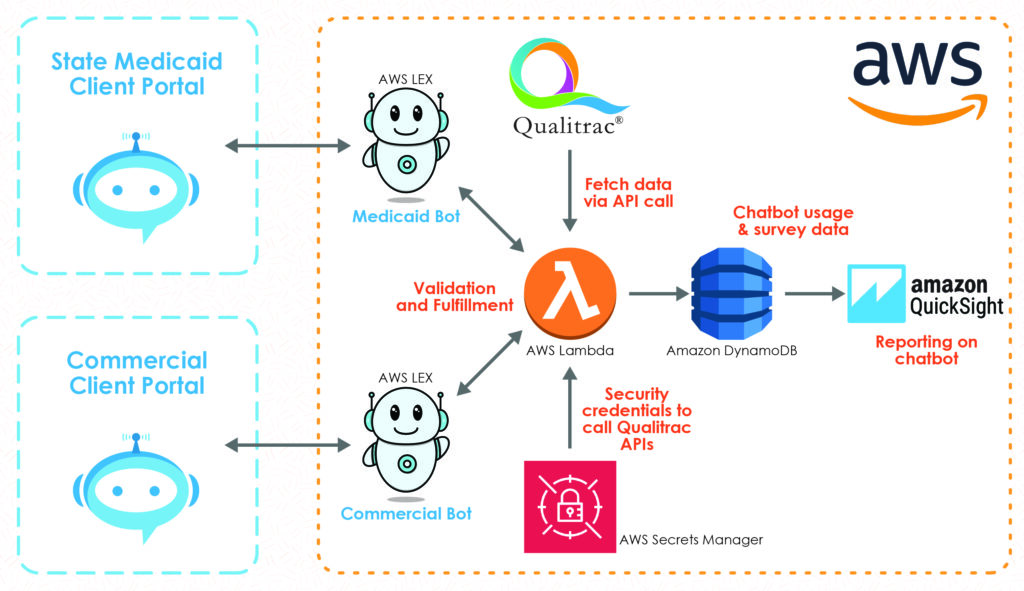
The workflow involving a chatbot for querying the status of prior authorization review goes as follows:
First, the chatbot is deployed on a public website that providers use to check the status of their patient’s prior authorization reviews. The chatbot collects the necessary data from providers and sends it to the back-end Lambda function. The Lambda function is responsible for performing both data validation and request fulfillment.
As part of the fulfillment operation, the Lambda function calls the Qualitrac® API to get the status of the prior authorization review. Once the Lambda function receives the necessary information, it relays it back to the chatbot. Additionally, on the backend, the Lambda function stores data related to chatbot usage and user experience. The data collected through the Lambda function could be used to gauge the effectiveness of chatbots for serving the prior authorization process using QuickSight reporting.
Privacy Concerns
 Natural Language Processing (NLP) has enabled chatbots to converse with humans in a more natural way than ever before. However, with the increased usage of NLP-enabled chatbots, concerns around data privacy have arisen. The chatbots use large amounts of data to learn and improve their responses, which may include personal information such as names, contact information, and even health records. Therefore, there are valid concerns regarding the safety and privacy of such information.
Natural Language Processing (NLP) has enabled chatbots to converse with humans in a more natural way than ever before. However, with the increased usage of NLP-enabled chatbots, concerns around data privacy have arisen. The chatbots use large amounts of data to learn and improve their responses, which may include personal information such as names, contact information, and even health records. Therefore, there are valid concerns regarding the safety and privacy of such information.
To address these concerns Telligen has implemented strict privacy policies and guidelines for chatbot development. Such guidelines include restricting the collection of unnecessary data and ensuring that data is stored securely. Additionally, chatbots could be designed to prompt users for permission before collecting any sensitive information. Users must be informed of what data the chatbot is collecting and how it will be used. Furthermore, Telligen is implementing features such as automatic data deletion after a certain period to ensure that personal information is not stored indefinitely.
Another way to address privacy concerns is to use end-to-end encryption. End-to-end encryption ensures that only the sender and recipient of a message can read it, and not any intermediaries, including chatbot providers. This means that the chatbot provider cannot read the messages exchanged between the user and the chatbot. End-to-end encryption can help users feel more secure in sharing personal information with chatbots.
Benefits
There are several benefits of using NLP-enabled chatbots in healthcare for prior authorization reviews. First, NLP-enabled chatbots can save time for healthcare providers by providing quick and easy access to information. Healthcare providers can check the status of prior authorization requests without having to navigate complex systems or wait on hold for extended periods.
Second, NLP-enabled chatbots can improve the accuracy of prior authorization reviews by eliminating the potential for human error. NLP-enabled chatbots can access and interpret data with high precision, reducing the risk of errors in the prior authorization process.
Finally, NLP-enabled chatbots can improve patient outcomes by ensuring that healthcare providers have access to up-to-date information on the status of prior authorization requests. This can help providers make informed decisions about patient care and avoid delays in treatment.
Conclusion
In conclusion, NLP-enabled chatbots have the potential to revolutionize the way healthcare providers check the status of prior authorization reviews. By providing quick and easy access to information, improving accuracy, and improving patient outcomes, NLP-enabled chatbots can help healthcare providers deliver high-quality care more efficiently. As the healthcare industry continues to embrace technology, it is likely that we will see an increasing use of NLP-enabled chatbots in various applications.
